Blog: Information from unexpected sources | David Barber
David Barber, Trainee Advanced Practitioner / Respiratory Physiotherapist
Knowsley Community Respiratory Service
I’m certain we have all experienced that moment, when information not sought drops into view. This happened to me (Rather fortuitously as I needed an area to study as part of a university project) recently, when completing an ambulatory oxygen assessment with a patient on EMIS, an electronic patient record and on completing the patient assessment document. On hitting the enter key for “Home Oxygen Order Form Completed”(something not usually entered under the active problem list), a bright red interaction warning box popped up – which was one of the last things I had expected to see at this point in proceedings, warning that Metformin was contra-indicated with respiratory failure.
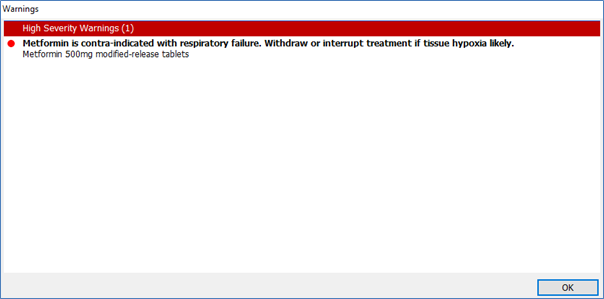
This sent me down something of a rabbit hole, in attempting to ascertain what was actually going on. UK oxygen guidelines make no mention of Metformin when considering oxygen as a therapy, but there are cautions within diabetic metformin guidance (Within the BNF & NICE), which do – the potential risk being flagged is that of anyone at risk of lactic acidosis, including those at risk of tissue hypoxia. Although further reading appears to indicate that there is no consensus on the actual risk, the fact remains that medication guidelines exist.
Is this widely known?
Talking with colleagues at a local level, and former colleagues across the north west, it appears that very few clinicians were aware of this risk – partly due to the non-diabetic speciality in which we work (And therefore lack of oxygen based metformin guidelines), but also the nature of the electronic documentation itself. Within our local system, although oxygen is documented, it is not done within the medications section of the record, and so appears to bypass the usual interaction warning mechanisms.
So now what?
Looking at our local population, just over 12% of patients assessed for long term oxygen with a PaO2 measured at less than 8.0 kPa were also prescribed Metformin concurrently, and whilst some of these would go on to use oxygen to correct this, there is a cohort of patients who either decline oxygen therapy, or are unsuitable (for example the current smoker) – who would all be at risk of tissue hypoxia, and therefore a potential greater risk of developing Metformin associated lactic acidosis.
The question of what to do with this information then developed – as a non-diabetic specialist service, it would not be appropriate to suggest adjustments in diabetic therapy by ourselves, but equally, bombarding overstretched primary care colleagues with this information may not be appropriate either. It was agreed locally, to highlight this information to primary care colleagues where patients have demonstrated respiratory failure, but oxygen therapy is not commenced, to allow for further optimisation of diabetic care where possible.
Moving forwards, and continuing to look for Metformin use within our patients, this does raise the suspicion that other such interactions / cautions exist, but due to historical ways of working (In this case documenting oxygen in a different manner to other medications) or the nature of specialist services potential lack of knowledge in other areas, these remain to be “discovered” by the curious.
PCRS Guest BlogsWe welcome guest blogs from our members or the wider respiratory care community that inform, educate and/or express opinion on respiratory matters. Views expressed in guest blogs are those of the author and do not necessarily reflect the policy or opinion of PCRS. If you have an idea for a blog or a podcast please do get in touch. |